
TRT and Fertility: What Men Need to Know Before Starting Treatment
TRT and Fertility: What Men Need to Know Before Starting Treatment Testosterone replacement therapy is one of the most effective
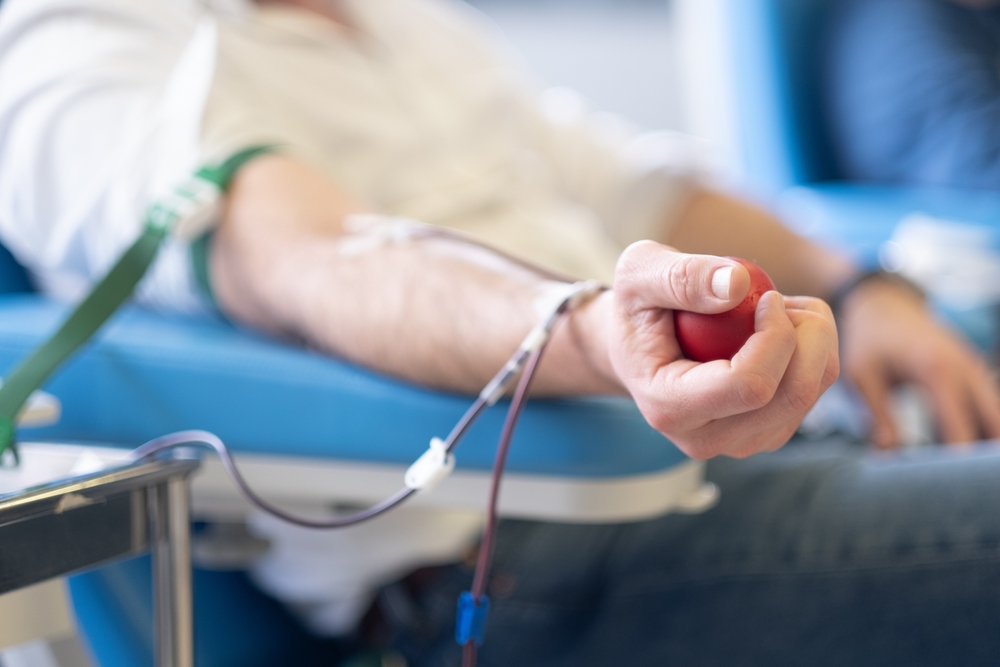
If you are considering testosterone replacement therapy, one of the first things your provider will tell you is that treatment cannot begin without lab work. This is not a formality. Blood work is the foundation of safe, effective TRT from the first appointment through every stage of ongoing treatment.
Understanding what tests are ordered, what they measure, and why they matter gives you a much clearer picture of what to expect from the process. It also helps you recognize when your monitoring is being done properly and when it is not.
This guide covers the essential TRT blood work required before starting treatment, what gets monitored during treatment, what the results mean, and how to interpret them in context with your symptoms.
TRT is a hormone therapy that produces real physiological changes throughout the body. Done properly, it improves energy, mood, body composition, sexual function, and overall quality of life. Done improperly, without adequate baseline testing and ongoing monitoring, it can cause or worsen a range of health issues including polycythemia, elevated estrogen, liver stress, and cardiovascular strain.
Blood work serves two essential purposes in TRT management. First, it confirms the diagnosis. Low testosterone is a medical condition defined by measurable hormone levels, not just symptoms alone. A provider cannot responsibly prescribe TRT without objective evidence that testosterone is actually low. Second, it provides the baseline data needed to monitor how your body responds to treatment and catch any problems before they become significant.
Any provider who offers TRT without requiring comprehensive pre-treatment lab work is not practicing responsible medicine. The same applies to ongoing treatment without regular monitoring panels.
Before any testosterone prescription is written, a thorough baseline panel is required. Here is what that panel typically includes and why each test matters.
This is the primary diagnostic test. Total testosterone measures the overall amount of testosterone circulating in your blood, including testosterone that is bound to proteins and testosterone that is freely available to the body.
Testing should be done in the morning, ideally between 7 and 10 a.m., because testosterone levels follow a circadian rhythm and are highest earlier in the day. A single low reading is generally confirmed with a second test before a diagnosis is made.
According to guidelines from the American Urological Association, a total testosterone level below 300 nanograms per deciliter is the threshold typically used to define testosterone deficiency, though clinical context and symptoms always accompany the number.
Free testosterone measures only the portion of testosterone that is not bound to proteins and is therefore biologically active and available to tissues. Some men have total testosterone levels within the normal range but free testosterone levels that are low, which can still produce symptoms of deficiency.
This test is particularly important for men who have symptoms consistent with low testosterone but a total testosterone reading that falls in the borderline range.
These two hormones, produced by the pituitary gland, signal the testes to produce testosterone and sperm respectively. Measuring LH and FSH helps providers determine the cause of low testosterone.
If LH and FSH are low alongside low testosterone, the problem likely originates in the pituitary or hypothalamus rather than the testes. This is called secondary hypogonadism. If LH and FSH are high with low testosterone, the testes themselves are not responding adequately. This is called primary hypogonadism. The distinction matters because it affects which treatment options are most appropriate.
Estradiol is the primary form of estrogen in men. Testosterone naturally converts to estradiol through a process called aromatization. Men need some estradiol for bone health, cardiovascular function, and mood regulation, but levels that are too high can cause symptoms including water retention, breast tissue development, mood changes, and reduced libido.
Baseline estradiol levels help providers understand your hormonal balance before treatment and inform decisions about whether an aromatase inhibitor may be needed during TRT.
A complete blood count measures red blood cells, white blood cells, and platelets. The most important value for TRT management is hematocrit, which measures the proportion of blood volume made up of red blood cells.
Testosterone stimulates red blood cell production, and elevated hematocrit is one of the more common side effects of TRT. If hematocrit rises too high, the blood becomes thicker, increasing the risk of clotting events. Baseline CBC establishes where your levels are before treatment begins so any increase can be identified and managed.
PSA is a protein produced by the prostate gland. Elevated PSA can indicate prostate inflammation, benign prostatic hyperplasia, or prostate cancer. Baseline PSA is required before starting TRT because testosterone can stimulate prostate tissue, and providers need to know your starting level before treatment to monitor for any significant changes.
According to guidelines referenced by the Endocrine Society, men with known or suspected prostate cancer are generally not candidates for TRT, making PSA screening an essential pre-treatment step.
A comprehensive metabolic panel assesses kidney function, liver function, blood sugar, and electrolytes. Liver function is particularly relevant because some forms of testosterone, specifically oral formulations, can affect liver enzymes. The CMP also provides context for overall metabolic health that informs treatment planning.
A lipid panel measures cholesterol and triglyceride levels. Testosterone therapy can affect lipid profiles, and a baseline reading allows providers to monitor for any changes that may require dietary or medical management during treatment.
Starting TRT is not a one-and-done event. Responsible ongoing management requires regular blood work at defined intervals throughout treatment. The following tests form the core of a standard TRT monitoring panel.
After starting TRT, testosterone levels are typically rechecked at four to six weeks to assess whether the dose is producing the desired result. Levels that are too low may indicate that the dose needs to be increased. Levels that are too high may require a reduction to avoid side effects. Once levels are stable and optimal, testing frequency typically shifts to every three to six months.
Hematocrit is one of the most important values to monitor during TRT because of the risk of polycythemia, a condition where the blood has too many red blood cells. Most providers check hematocrit at three months after starting treatment and then every six months once levels are stable.
If hematocrit rises above approximately 54 percent, treatment is typically paused or the dose is reduced until levels normalize. In some cases, therapeutic phlebotomy, which is essentially a controlled blood donation, is used to manage elevated hematocrit.
Estradiol is monitored throughout treatment because testosterone converts to estradiol through aromatization, and this conversion increases as testosterone levels rise. Some men convert at higher rates than others, making regular estradiol monitoring essential for catching imbalances early.
Symptoms of high estradiol during TRT include water retention, mood changes, breast tenderness, and reduced sexual desire. If estradiol rises significantly, providers may recommend an aromatase inhibitor to manage the conversion.
PSA is typically rechecked at three to six months after starting TRT and then annually. A significant rise in PSA during treatment warrants further evaluation, including potential referral to a urologist.
Monitoring LH and FSH periodically during TRT helps confirm that the hypothalamic-pituitary-gonadal axis is responding as expected and provides information relevant to fertility considerations for men of reproductive age.
One of the most common questions men have about managing TRT through a telehealth provider is how blood work gets done without an in-person clinic visit.
The process is straightforward. Your telehealth provider sends a lab requisition to a facility such as LabCorp, which has locations across the country. You visit your nearest location for the blood draw, which takes a few minutes. Results are sent electronically to your provider, who reviews them and follows up with you virtually to discuss findings and any adjustments needed.
This model provides the same quality of monitoring as an in-person clinic without requiring travel to a specialized facility. For men in states where in-person hormone clinics are not easily accessible, telehealth-based TRT monitoring is a practical and medically sound alternative.
If you are located outside of Maryland and are interested in accessing TRT through telehealth, out-of-state consultation options are available for residents of several states with the same standard of care and monitoring.
Most providers check labs at four to six weeks after starting treatment, then at three months, and then every six months once levels are stable. If dose adjustments are made, additional testing is scheduled to confirm the new dose is producing the right result. The exact schedule varies by provider and individual response.
If blood work shows testosterone levels above the optimal range, your provider will reduce your dose and recheck levels after a few weeks. Very high testosterone levels can increase the risk of side effects including elevated hematocrit, mood changes, and excess estradiol conversion. This is why regular monitoring is essential rather than optional.
Most providers include PSA as part of the pre-treatment panel regardless of age, because it establishes a baseline. The ongoing significance of PSA monitoring increases with age, but having a baseline before starting TRT is important for all men.
Your provider will specify which lab to use based on the requisition they send. LabCorp is commonly used by telehealth providers because of its nationwide network. You do not need to visit a specialized clinic. Any local LabCorp location can process the draw and send results directly to your provider.
Borderline total testosterone levels do not automatically rule out treatment. Free testosterone, symptoms, and overall clinical picture all contribute to the diagnosis. Some men with total testosterone in the low-normal range have free testosterone levels that are genuinely low and experience significant symptom relief from treatment. This is a conversation to have with your provider based on your full panel. You can also use the ADAM Questionnaire for Men as a structured way to document your symptoms before your consultation.
Coverage varies significantly depending on your insurance plan. Many plans cover diagnostic blood work but may not cover monitoring labs for treatments they classify as elective. For patients on a direct pay model, lab costs are a straightforward out-of-pocket expense that is typically clearly communicated upfront.
TRT blood work is not bureaucratic overhead. It is the clinical foundation that makes testosterone replacement therapy safe, effective, and appropriately personalized to your individual physiology. Understanding what gets tested and why helps you participate more actively in your own care and recognize when your treatment is being managed responsibly.
If you are ready to take the first step toward evaluating your testosterone levels and understanding your options, a telehealth consultation with a qualified provider is the most accessible way to get started. Learn more about testosterone replacement therapy and what the process looks like from initial consultation through ongoing monitoring.
This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare provider before starting, stopping, or changing any medication or treatment plan.

TRT and Fertility: What Men Need to Know Before Starting Treatment Testosterone replacement therapy is one of the most effective
Semaglutide vs Tirzepatide for Weight Loss: What Is the Difference? If you have been researching prescription weight loss medications, you

How to Maintain Weight Loss After a Medical Program Ends Reaching your weight loss goal is a real achievement. It

How Long Does TRT Take to Work? A Realistic Timeline of What to Expect One of the most common questions
Currently only accepting new clients from: New Mexico, Utah, Minnesota, Maryland, Virginia, Delaware, Colorado, West Virginia, Arizona, Iowa, Florida, Nevada, and Connecticut.